In medical practice, certain signs and symptoms provide crucial information about a patient’s cardiovascular health. One such sign is jugular venous distention, often abbreviated as JVD. Jugular venous distention is an important clinical finding that can indicate underlying heart or circulatory problems. Understanding what jugular venous distention is, how it occurs, how it is assessed, and its implications can help patients and healthcare professionals recognize potential health issues early. This topic provides a detailed explanation of jugular venous distention, its causes, assessment techniques, and significance in clinical medicine.
Definition of Jugular Venous Distention
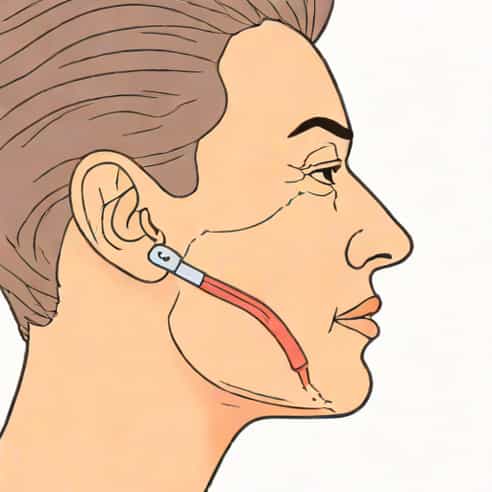
Jugular venous distention refers to the visible enlargement or bulging of the jugular veins in the neck, which results from increased pressure in the right atrium of the heart. The jugular veins are major veins that carry blood from the head back to the heart. When the pressure in the right side of the heart rises, blood flow is impeded, and the jugular veins become distended. Clinicians often use jugular venous distention as a non-invasive indicator of increased central venous pressure, which can reflect heart dysfunction or fluid overload.
Anatomy of the Jugular Veins
The jugular veins consist of the internal and external jugular veins, which run along the sides of the neck. The internal jugular vein is the primary vein assessed for jugular venous distention because it directly communicates with the right atrium of the heart. The external jugular vein can also become visibly enlarged in some cases, but the internal jugular vein provides a more accurate reflection of central venous pressure. Understanding the anatomy is important for correctly identifying and assessing JVD.
Causes of Jugular Venous Distention
Jugular venous distention can occur due to several underlying medical conditions that affect the heart or circulation. Some common causes include
- Right-sided heart failure, which prevents the heart from effectively pumping blood to the lungs.
- Constrictive pericarditis, a condition in which the pericardium becomes stiff and restricts heart movement.
- Cardiac tamponade, where fluid accumulation around the heart compresses it and increases venous pressure.
- Pulmonary hypertension, which raises pressure in the pulmonary arteries and right side of the heart.
- Superior vena cava obstruction, which can lead to impaired blood flow from the upper body to the heart.
Clinical Significance of Jugular Venous Distention
Jugular venous distention is clinically significant because it provides a visual clue about the pressure inside the heart and the circulatory system. It is commonly used in the assessment of heart failure, fluid overload, and other cardiovascular conditions. Detecting JVD can help healthcare professionals determine the severity of a patient’s condition, monitor treatment effectiveness, and decide on interventions such as diuretics, fluid restriction, or more advanced therapies. It is a simple but valuable bedside tool in cardiology and emergency medicine.
How to Assess Jugular Venous Distention
Assessing jugular venous distention requires proper patient positioning, observation, and sometimes measurement. The standard procedure includes
- Positioning the patient at a 30- to 45-degree angle, with the head slightly turned away from the examiner.
- Identifying the top of the venous pulsation in the neck, usually along the right internal jugular vein.
- Measuring the vertical height of the pulsation above the sternal angle, which provides an estimate of central venous pressure.
- Observing changes during respiration, as jugular venous pressure may vary with breathing.
Experienced clinicians can often recognize JVD visually, but measurement provides more objective data, especially in complex cases.
Symptoms Associated with Jugular Venous Distention
While JVD itself is a sign rather than a symptom, it is often accompanied by symptoms of the underlying condition causing it. Common associated symptoms include
- Shortness of breath or difficulty breathing, especially in heart failure.
- Swelling in the legs or ankles due to fluid retention.
- Fatigue or weakness caused by reduced cardiac output.
- Palpitations or irregular heartbeats in some cases of heart disease.
Diagnosis and Related Tests
In addition to visual assessment, jugular venous distention may be evaluated using diagnostic tools. These can include
- Echocardiography to assess heart structure and function.
- Chest X-rays to evaluate heart size and pulmonary congestion.
- Electrocardiograms (ECG) to detect heart rhythm abnormalities.
- Blood tests, including BNP (B-type natriuretic peptide), to assess heart failure.
Combining JVD assessment with these diagnostic tests improves accuracy in determining the severity and cause of cardiovascular problems.
Treatment and Management
The management of jugular venous distention depends on addressing the underlying cause. For example, in patients with right-sided heart failure, treatments may include diuretics to reduce fluid overload, lifestyle changes, and medications to improve heart function. In cases of pericardial tamponade, emergency procedures may be required to remove excess fluid. Pulmonary hypertension may be treated with medications to reduce blood pressure in the lungs. Effective management of the underlying condition usually results in a reduction of JVD, highlighting its usefulness as a monitoring tool.
Importance in Emergency Medicine
Jugular venous distention is particularly important in emergency and critical care settings. It can serve as an immediate visual cue for clinicians to identify patients at risk of severe heart failure, cardiac tamponade, or fluid overload. Quick recognition of JVD can lead to faster interventions, potentially saving lives. Its simplicity and accessibility make it a vital component of physical examinations in urgent situations.
Jugular venous distention is a key clinical sign that provides important information about heart and circulatory function. Defined as the visible enlargement of the jugular veins due to increased right atrial pressure, it can indicate conditions such as heart failure, cardiac tamponade, and pulmonary hypertension. Understanding the anatomy, causes, assessment techniques, and clinical significance of JVD allows healthcare providers to make informed decisions about diagnosis and treatment. Recognizing and properly evaluating jugular venous distention remains a fundamental skill in medicine, offering insight into a patient’s cardiovascular health and guiding effective interventions.